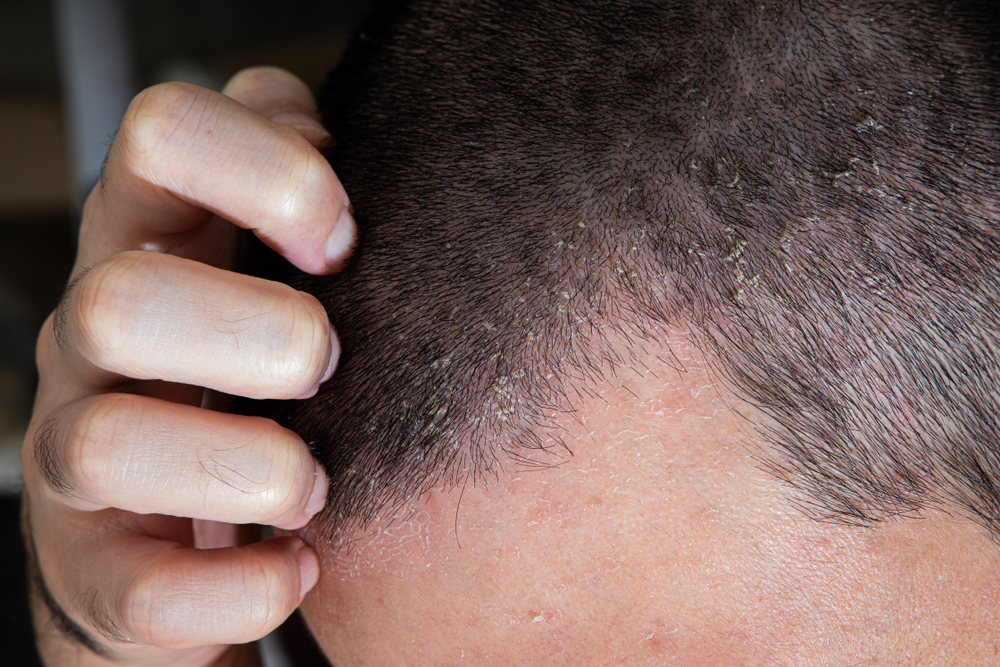
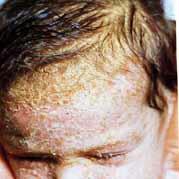
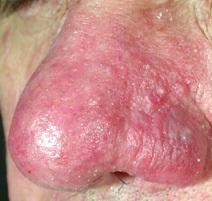
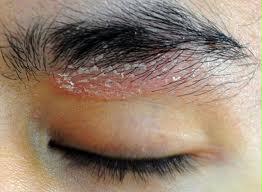
Grey hair
In the trichological field, with the passing of age hair whitening is seen to follow the greying process of the hair on the scalp (called grey hair). Hair becomes grey (white) following a natural biological aging process of the melanocytes, which are the cells tasked with coloring hair.
In the majority of people, the first grey hairs appear around 35/40 years of age in women and around 30/35 in men.

 Italiano
Italiano  Português
Português  Français
Français  Español
Español